Personalised cancer vaccine shows promising results in clinical trial.
A new study has shown that a personalised cancer vaccine that targets mutations within a patient’s tumor can prevent its regrowth, offering a significant milestone for the cancer vaccine field. The study, reported at the annual meeting of the American Association for Cancer Research, revealed that patients who received a personalised vaccine along with an immunotherapy drug were more likely to remain free of cancer 18 months later than those who did not receive the vaccine. This offers the first clear evidence that a vaccine tailored to genetic changes in a person’s tumor can prevent its regrowth.
Traditional cancer vaccines aim to teach the immune system’s T cells to attack a tumor by exposing them to a protein, or antigen, that pokes out from a cancer cell. But most vaccines have failed to work effectively because the same antigens found on tumors also appear on normal cells.

However, in recent years, as DNA sequencing costs have decreased, some scientists have turned to sequencing the mutations in a patient’s tumor, then creating a vaccine to deliver a few of the corresponding mutated proteins, known as neoantigens, which are found only on the tumor cells.
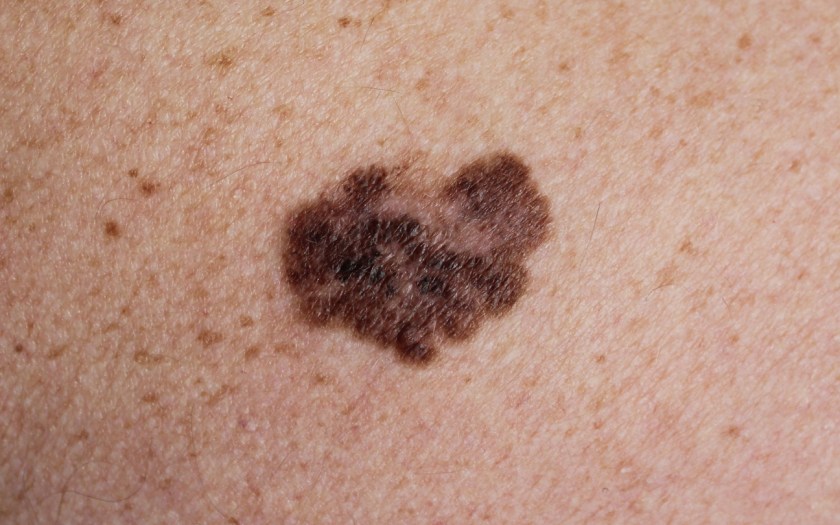
Testing In Melanoma Patients
Merck and Moderna conducted a randomised trial for patients who had advanced melanoma that had spread to lymph nodes and sometimes other sites but that had been surgically removed. All participants received a checkpoint inhibitor drug that blocks a crucial protein from enabling tumors to evade T cells, with two-thirds also receiving vaccine infusions every 3 weeks for about 4 months. The cancer vaccine delivered messenger RNA (mRNA) wrapped in lipid nanoparticles into cells, instructing them to make a protein—in this case, up to 34 tumor neoantigens per patient.
Study findings
In December 2022, the companies reported that patients receiving the vaccine were 44% less likely to die or have a recurrence of their cancer. 84 of the 107 patients, or 79%, were still in remission after 18 months, compared with only 31 of 50 (62%) patients who got the checkpoint inhibitor alone. The vaccine worked regardless of how many mutations the person’s melanoma tumor had, suggesting it could work for cancer types with fewer mutations. This is encouraging as such cancers tend to resist immunotherapy drugs.
A larger study is set to start later this year, aiming to confirm the results of the trial and reveal whether the vaccine extends patients’ lives. Such results could encourage regulators to approve the vaccine. As more details emerge, including evidence that patients who did well made T cells specific to the neoantigens and did not just get an immune boost from the vaccine’s nanoparticles, researchers hope to gain a better understanding of the efficacy of personalised cancer vaccines.
Read SPA+CLINIC’s latest issue here:
There are 5 ways you can catch up with SPA+CLINIC
- Our quarterly print magazine, delivered to your door. Subscribe here.
- Our website, which is updated daily with its own completely unique content and breaking news.
- Our weekly newsletter – free to your inbox! Subscribe here.
- Our digital magazine – click here to view previous issues.
- Our social media – see daily updates on our Instagram, Facebook & Linkedin