It may not be as common as other adverse events, but FIA needs to be part of your informed consent.
Temporary and permanent alopecia is an underreported (and often unknown) aesthetic adverse event that has been documented following multiple cosmetic injectable procedures including soft tissue fillers, deoxycholic acid, mesotherapy, and even botulinum toxin. Filler Induced Alopecia (FIA) is becoming increasingly recognised, particularly with the rise of temple and forehead treatment. Currenting the cause is said to be related to vascular compromise, leading to tissue inflammation, hypoxia and in some cases necrosis and scarring. This in turn leads to a premature termination of the anagen phase. Onset time for FIA is documented to occur at around two weeks following filler, and whilst many patients experience temporary hair loss (often taking months to achieve resolution), it is important to note that patients experiencing necrosis and scarring are unlikely to achieve full resolution.
Why is FIA only now being recognised?
In aesthetic medicine, our knowledge of facial ageing and anatomy is continuously growing, and as such we change or adapt our techniques. So, whilst FIA has been reported in the literature (and likely occurring in higher numbers) for the last decade, it was considered rare as it was most commonly seen following forehead filler treatments; an area considered high-risk and usually performed by a smaller group of highly experienced practitioners.
However, recent literature has emerged with respect to temporal hollowing and how ageing of this region affects the mid and lower face. In addition, articles have discussed the individual temporal layers, and how filler placement within specific planes impacts patient’s aesthetic results. Clearly this research is beneficial in helping practitioners understand the strengths and limitations of filler treatments by showcasing a direct correlation to the anatomical layers, as well as ensuring practitioners do not continue to overfill the mid and lower face to achieve greater “lift”. It also advocates using lower more targeted volumes to achieve more impactful results, thereby ensuring more natural and anatomically oriented aesthetic results.
With this advancement in research, we have seen a rapid trend towards using a larger gauge cannula (22g – 25g) in the superficial temporal layers to achieve a lift of the mid and lower face. Whilst the superficial temple technique has been around for many years, its uptake was not so popular given its close proximity to temporal vessels; in particular the superficial temporal artery. However, now that recent literature has highlighted the aesthetic benefits of the superficial technique, it seems practitioners are now far more comfortable treating in the plane they once felt was far too risky.
What is AMET’s experience with vascular compromise and FIA?
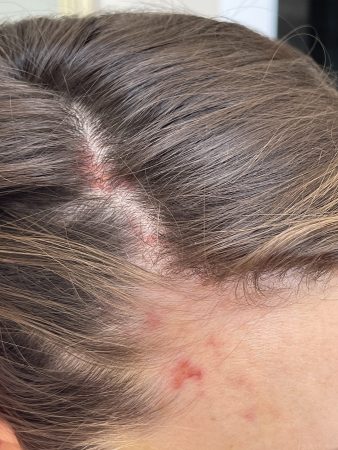
In the last eight months, AMET has had five cases of vascular compromise of the superficial temporal artery (and/or branches of STA) following superficial temple filler with large gauge cannulas. In all of the cases, the patients experienced symptoms including pain, discolouration, blisters and signs of impending necrosis extending from the temple into the scalp. Only one case presented with immediate blanching during the procedure, with all other cases having delayed clinical presentation, even up to four days later.
These cases have highlighted to us an urgent need to promote more awareness of this complication, as well as the need to ensure practitioners include filler induced alopecia as part of their informed consent. In addition, there has been a 2021 case report by Schelke and colleagues discussing a patient that experienced diffuse alopecia following a lateral zygoma filler treatment. Needless to say, filler induced alopecia should become a standard risk discussed during patient consultation for any filler treatment.
How do we measure Risk Vs Benefit in Aesthetics?
We ALL want to do right by the patient and we are all in this to help our patients feel better. However we ALL need to understand that we are NEVER safe. Yes, studies have shown larger gauge cannulas require more force to enter vessels, however this is directly impacted by the anatomical location and fixation of the vessel itself. Anatomically there is very little “wiggle room” in the upper face, which means vessels are less likely to be pushed aside, even with a 22g cannula. On top of this, injection force is a subjective interpretation by the practitioner, with recent literature highlighting anatomical variances in the temple that directly anastomose with the ophthalmic circulation.

If we want to accurately assess treatment risk in aesthetics we must first think outside the box. We must question everything we have been taught and everything we have read. As a united industry we need to work towards standardising our risk assessment procedures to match that of other health care settings. Without this unified approach, we will always run the risk of letting our desire to achieve the “best” aesthetic result cloud our ability to assess treatment risk. Ultimately, we all need to presume we are never safe (needle or cannula), believe we are intravascular when injecting, accept that our anatomy knowledge is still limited, and when a complication occurs, we must be well prepared to manage and support our patients.
For information on how to become an AMET member, please visit www.aestheticmet.com or email clinical@aestheticmet.com.
This article originally appeared in SPA+CLINIC Vol 91.
Read SPA+CLINIC’s latest issue here:
There are 5 ways you can catch up with SPA+CLINIC
- Our quarterly print magazine, delivered to your door. Subscribe here.
- Our website, which is updated daily with its own completely unique content and breaking news.
- Our weekly newsletter – free to your inbox! Subscribe here.
- Our digital magazine – click here to view previous issues.
- Our social media – see daily updates on our Instagram, Facebook & Linkedin