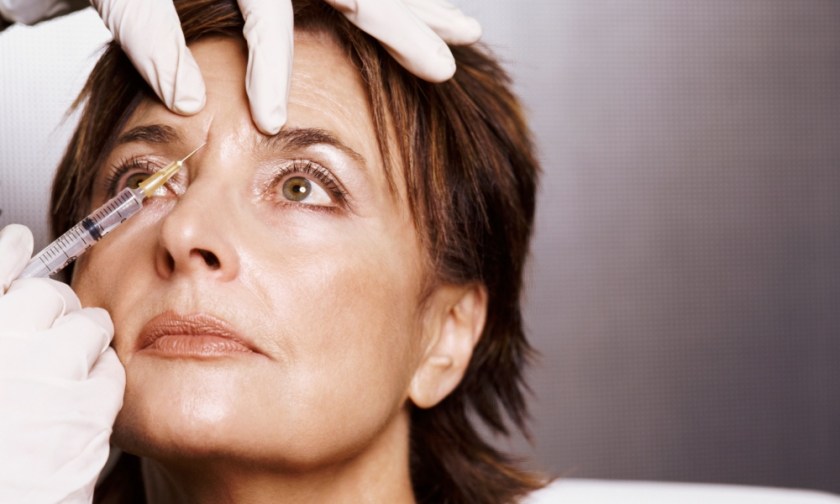
Blindness, strokes, even death … when injectables go wrong. And the steps to prevent tragedy. By Jenni Gilbert.
The doctor who stumbled on the skin-smoothing effects of Botox in 1987 stunned a conference in Canada last week by revealing nearly 100 people worldwide have been left blind after having facial dermal fillers.
Highlighting the danger at the World Congress of Dermatology conference in Vancouver, opthamologist Professor Jean Carruthers told delegates: ‘Ninety eight patients lost vision in one or both eyes after having facial filler mistakenly injected into a blood vessel, leading to blockage of crucial arteries supplying blood to the eyes.’
She added that in a quarter of the 98 cases, dermal filler – whether it be a hyaluronic acid formula or autologous (ie. the patient’s own) fat – had made it into the brain, with some patients suffering strokes as a result.
Although I have been having anti-wrinkle injections and dermal fillers for many years, I was unaware of this risk until only a few weeks ago when I requested Sydney cosmetic physician Dr Naomi McCullum inject filler into the glabellar lines (between the eyebrows) as anti-wrinkle formulas are not doing the trick they once were for me.
She explained that injecting filler anywhere around the eyes can be a risky business unless performed by a highly trained and experienced injector.
Because the skin is much thinner in that area than elsewhere on the face, the risk of injecting a bit too deeply and hitting a blood vessel cannot be ignored. (This does not apply to anti-wrinkle injections, however, as these are only shallow penetrations.)
‘The vast majority of injectable outcomes are excellent, which is why they are so popular,’ says Dr McCullum. ‘However, dermal filler injection is a medical procedure, and decisions about it need to be taken seriously by the injector and the patient.
‘Injectors need to know their facial anatomy and where the more risky sites for injecting are, and how to reduce the risk of complications.
‘We’re not talking about temporary bruising or swelling here, which are the more typical complications of fillers.
‘Blindness, although rare, would be devastating. Patients need to be aware of the risks, and weigh them against the benefits. This will help them decide whether going ahead with the procedure is right for them.’
Dr McCullum’s comments reinforce the need for any salon, spa or clinic owner bringing doctor or nurse injectors into their business on a permanent or semi-regular basis to be absolutely confident in these medicos’ qualifications, skills and experience, and also to be aware of the requirements, implications and ramifications of offering injectables on your business premises to clients.
A good first step would be to contact a reputable medical body such as the Australasian Academy of Cosmetic Surgery (ACCS) or the Cosmetic Physicians Society of Australasia (CPSA).
Indeed, ACCS president Dr Soo-Keat Lim is deeply concerned the lack of regulations governing the practice of cosmetic surgical and medical procedures in Australia (not specifically injectables, but also non-surgical treatments such as use of lasers).
‘This has resulted in poorly trained practitioners whether they are doctors, nurses or dentists projecting themselves into the public arena claiming to be experts in cosmetic medical practice, thus putting the patients in harm’s way,’ says Dr Lim.
‘The ACCS wishes to see the relevant authorities introduce regulations that will ensure that any practitioner in cosmetic surgical and cosmetic medical procedures is appropriately trained in the procedures that they are working in.
‘For example, just because you are a doctor or a nurse and you have been trained to give injections to your patients does not mean that you are already qualified or sufficiently trained to give anti-wrinkle or dermal filler injections.
‘The ACCS has courses that will train medical practitioners to reach the appropriate level of expertise for them to work safely and expertly in cosmetic medical practice.
‘The ACCS is also working closely with the College of Nursing to provide courses that will upgrade their skills in the cosmetic procedures that they are presently working in.’
The improper use of dermal fillers to treat frown and laugh lines that can cause retinal artery occlusion (RAO) and permanent blindness was first brought to light in 2012 in a South Korean study led by Dr Se Joon Woo, from Seoul National University’s Bundang Hospital in Seongnam, and published in the American Journal of Ophthalmology.
The research team found that use of autologous fat yielded significantly worse outcomes than hyaluronic acid and collagen injections.
‘Patients should be aware of the possibility of development of retinal/ophthalmic artery occlusion and if RAO develops, the visual prognosis is poor,’ Dr Woo said.
In Vancouver last week, Prof Carruthers told conference delegates: ‘Often the commonest filler to be used mid-face and around the eyes is autologous fat.
‘And you can’t get rid of fat once it’s in an artery. It’s there – you can’t dissolve it. It’s an utter disaster.’
www.drnaomi.com.au; www.accs.org.au; www.cosmeticphysicians.org.au